When your doctor says the words “stage 4 blood cancer”, it can feel overwhelming, as if the ground has shifted beneath you. The phrase "stage 4" carries so much weight and often brings to mind the most serious prognoses we associate with other cancers. But it's important to understand that for blood cancers, the term "stage 4" has a different meaning.
While this diagnosis is serious, it’s not automatically the end that many people fear. In the world of haematology, stage 4 is more of a description of where the cancer is, not necessarily how untreatable it is. In fact, many types of stage 4 blood cancers can be managed effectively with modern treatments, offering real possibilities for remission, control, and even a cure for some people.
So, let’s reframe what “stage 4” actually means for blood cancers. For solid tumours, like in the lung or breast, staging is like mapping a fire. A stage 4 diagnosis means the cancer has spread from its original location to distant parts of the body.
Blood cancers, on the other hand, are different from the very beginning. Because they originate in the blood or bone marrow, they're already part of the body's circulation system. Instead of thinking of it as a contained fire that spreads, imagine it more like a weather system; the cancer cells are already moving throughout the body's "atmosphere."
Therefore, "stage 4 blood cancer" doesn’t carry the same meaning as stage 4 in solid tumours. It simply confirms that the disease is widespread, something that is quite common and often expected with these types of cancers. It describes where the cancer is and does not mean that treatment options are limited or that hope is lost.
A stage 4 diagnosis is not the end of the road; it’s simply a starting point, giving your medical team the information they need to understand exactly where the cancer is and to build the right treatment plan for you. Think of it as a roadmap, not a final destination.
Here are some important things to keep in mind:
To give this some context, over 40,000 people are diagnosed with blood cancer each year in the UK, and an estimated 192,070 people in the US are expected to be diagnosed with leukemia, lymphoma, or myeloma in 2025. Advances in treatment and supportive care have improved outcomes and quality of life for many patients.
Your stage 4 diagnosis is a map that shows your doctors where to fight. It's the beginning of the conversation about your treatment journey, not the end of it.
Part of this journey involves understanding the specific blood cancer symptoms and the challenges you may face, as it helps you and your care team manage your health effectively.
This guide is here to give you a clear, realistic, and hopeful foundation for understanding what comes next.
When you first receive a diagnosis, one of the first things you’ll encounter is the concept of "staging". But it’s important to understand that staging is not a one-size-fits-all process. Doctors use different systems for different blood cancers, because each one behaves in its own unique way.
Take leukaemia as an example. Many leukaemias are not described using the familiar 1-to-4 scale, and some use their own disease-specific staging or phase systems. That’s because leukaemia starts in the bone marrow, where blood is made, so cancer cells are circulating throughout the bloodstream from the very beginning. In that sense, it is often considered widespread from day one.
So, instead of relying on traditional stage numbers, your medical team will focus on several key details that give them a much clearer picture for planning your treatment. They’ll look at:
These factors are often far more important for leukaemia than a simple stage number. If you’d like to dig deeper, you can read more about the importance of the bone marrow in the progression of leukaemia.
Unlike leukaemia, which is considered widespread from the start, lymphomas and multiple myeloma have very specific staging systems that your medical team will use to understand and map out the extent of the cancer and plan the best treatment for you.
For lymphomas, the most widely used method today is the Lugano classification, which is a modern update to the older Ann Arbor system. This system focuses mainly on location. In simple terms, it tracks where the lymphoma has spread in your body. Stage 4 blood cancer lymphoma means the cancer has spread beyond the lymph system to one or more organs, such as the liver, lungs, or bone marrow.
Staging acts as a roadmap for your medical team. It tells them not only where the cancer is, but also provides clues about how it might behave, which is essential for choosing the most effective treatment.
When it comes to multiple myeloma, doctors use a powerful tool called the Revised International Staging System (R-ISS). This system goes much deeper than just mapping where the cancer has spread. This system provides a more detailed picture of the disease and helps shape the most effective treatment plan.
Think of the Revised International Staging System (R-ISS) as a more detailed diagnostic profile. It combines several critical clues from your blood tests and genetic analysis to predict how the disease might progress.
Specifically, it measures the levels of two proteins, beta-2 microglobulin and albumin, along with an enzyme called lactate dehydrogenase (LDH). It also checks for high-risk genetic mutations inside the myeloma cells.
By pulling all this information together, doctors can classify myeloma into one of three stages, with a higher stage pointing to a more aggressive disease. Every one of these systems, whether for lymphoma or myeloma, is designed to give your medical team the precise, evidence‑based information they need to build a treatment plan that’s right for you.
When you’re told you have stage 4 blood cancer, one of the first words you’ll hear is “prognosis.” It’s a heavy word, and it’s completely natural to want to look up survival rates and statistics immediately. But it’s important to know what those numbers actually mean, and what they aren’t.
Think of statistics as a blurry, wide-angle photo of a very large crowd. They give you a general idea of what has happened to many people in the past, but they can’t tell you anything about the individual journey of each patient, their stories, or what their futures hold. Your prognosis is personal; it’s shaped by your specific circumstances, not just a number pulled from a chart.
The truth is, the outlook for advanced blood cancers can vary enormously from person to person. For some people, like those with certain lymphomas, the goal is often a complete cure. For others, the cancer might be treated more like a chronic illness, where the focus is on keeping it under control and maintaining a good quality of life for as long as possible.
So, if general statistics don't tell the whole story, what does? Your healthcare team pieces together a much more detailed picture of your situation by looking at several key factors that go beyond stage numbers.
These are the elements they’ll consider when talking with you about your treatment plan and what to expect:
Together, these factors create a personalised outlook that is far more meaningful than broad statistics. Your prognosis is not fixed; it evolves with your treatment journey and the unique details of your health profile.
There are genuine reasons to hold onto hope. Advances in research and treatment have led to remarkable progress. Mortality rates for many blood cancers have fallen significantly over the last decade in many parts of the world. For instance, in countries like the UK, deaths from leukaemia and Hodgkin lymphoma have seen notable decreases thanks to effective therapies and improved care strategies.
While this progress is changing lives, it’s important to acknowledge that access to the newest treatments is not always straightforward. Understanding the reality of unequal access to advanced cancer treatments is an important step in being your own best advocate.
Above all, nothing replaces an open and honest conversation with your oncology team. They can provide the clearest picture of your personal situation, explain which treatments are available to you, and help you navigate the options with confidence.
When you hear that blood cancer has reached stage 4, it’s understandable to feel overwhelmed. The good news is that even at an advanced stage, there are many effective treatments available. Your oncology team will work closely with you to create a plan that's tailored not just to the cancer itself, but also your overall health, values, and what matters most to you.
The purpose behind treatment for stage 4 blood cancer can differ from person to person. Broadly speaking, the goals usually fall into one of three main categories.
To help understand different approaches, this table breaks down the main goals of treatment for stage 4 blood cancer. Your doctor might recommend one or a combination of these, depending on your unique situation.
| Treatment Goal | Primary Aim | Commonly Used Therapies | Example Scenario |
|---|---|---|---|
| Curative | To completely remove the cancer and achieve a lasting remission. | High-dose chemotherapy, stem cell transplants, intensive targeted therapies. | A younger, fit patient with a specific type of lymphoma that responds well to aggressive treatment. |
| Control | To manage the cancer as a long-term condition, slowing its growth and keeping symptoms under control. | Lower-dose chemotherapy, maintenance targeted therapies, immunotherapy. | A patient with multiple myeloma where the goal is to keep the disease stable for as long as possible. |
| Palliative | To focus on improving quality of life by managing pain and other symptoms, without aiming to cure the cancer. | Low-dose radiotherapy for pain relief, medications for nausea or fatigue, psychosocial support. | A patient for whom intensive treatments are no longer effective or would cause more harm than good. |
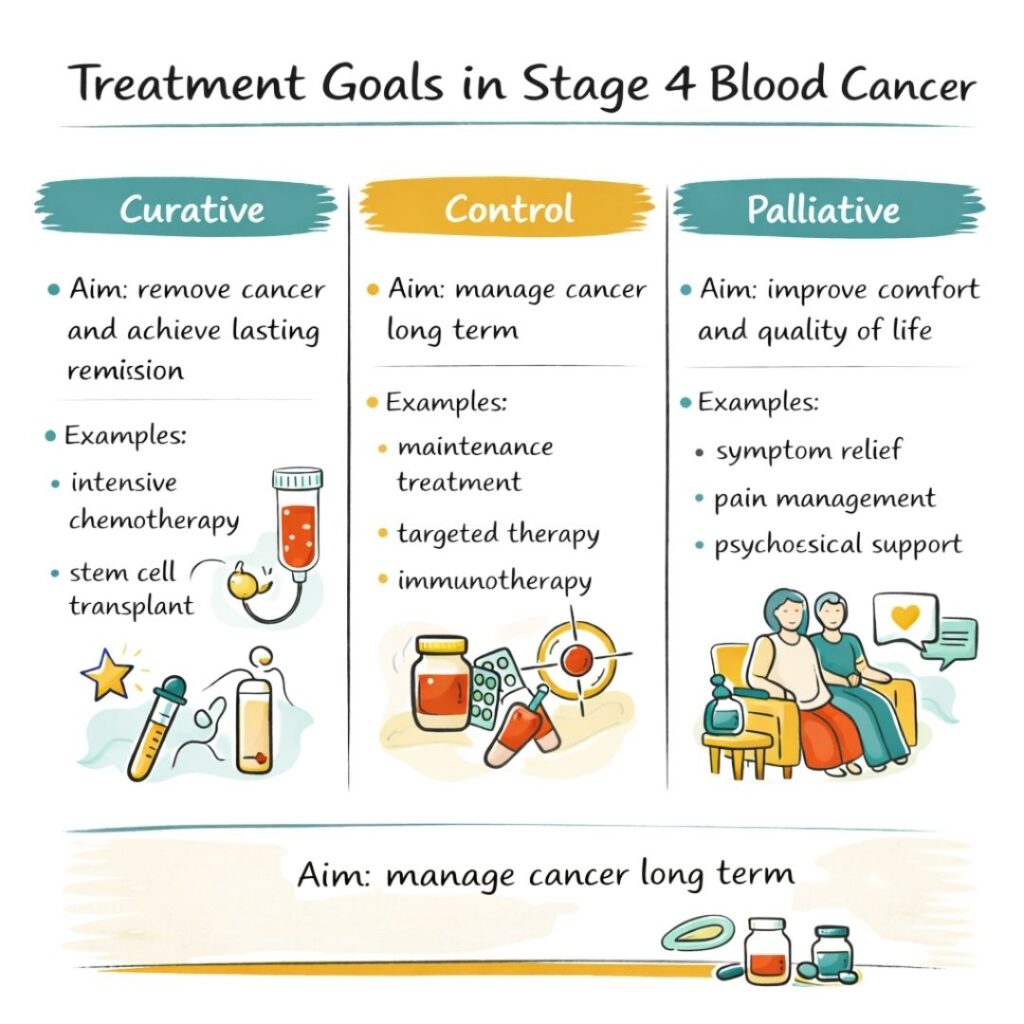
Understanding these different treatment goals is an important first step, as it helps you and your loved ones know what to expect from the treatment journey ahead with greater clarity and confidence.
When the goal is to directly fight the cancer, doctors have a wide range of effective tools available. The right combination of treatments will depend on the specific type of blood cancer, your general health, and even the genetic features of the cancer cells.
Chemotherapy remains a cornerstone of treatment. These powerful drugs are designed to target and kill cells that grow rapidly, a key feature of cancer. It is usually given in cycles, giving your body a chance to rest and recover between rounds.
Radiotherapy uses targeted, high-energy X-rays to destroy cancer cells in a specific area. This approach is especially effective for shrinking lymphoma tumours that are causing pain or pressure.
Stem cell transplant (sometimes called a bone marrow transplant) is a more intensive option. It allows doctors to give much higher, more effective doses of chemotherapy than would normally be possible. Afterwards, your blood-producing stem cells are restored using healthy cells that were either collected from you earlier or from a matching donor.
Together, these treatments form the backbone of approaches aimed at a cure or controlling stage 4 blood cancer, offering patients realistic paths toward remission or long‑term stability.
Alongside well-established treatments, cancer treatment has seen incredible progress in recent years. Two of the most significant developments are targeted therapies and immunotherapies.
Targeted therapies are precision drugs designed to exploit specific weaknesses in cancer cells. Think of them as a specially designed key that fits a unique lock on the cancer cell, shutting down its ability to grow while leaving most of your healthy cells alone.
Immunotherapy, on the other hand, takes a different approach. Instead of attacking the cancer directly, it strengthens your own immune system, teaching it to recognise and destroy cancer cells more effectively. If you're curious, you can learn more about how immunotherapy works and its growing importance in treatment.
One of the most talked‑about advances in immunotherapies is CAR-T cell therapy. This treatment involves taking your own immune cells, sending them to a specialised laboratory to be "re-engineered" into elite cancer-fighting specialists, and then infusing them back into your body to hunt down and destroy the cancer.
Finally, don’t hesitate to ask your doctor about clinical trials. These are research studies that test out new treatments or different ways of using existing ones. Taking part in a trial could give you access to the very latest medical advances before they become widely available and help push cancer care forward for future patients. Your doctor is the best person to guide you on whether a suitable trial is available and whether it’s the right option for your situation.
Living with stage 4 blood cancer is not just about the diagnosis itself; it’s about navigating the day-to-day reality of the illness and its powerful treatments. Protecting your quality of life by actively managing these symptoms and side effects is one of the most important things you can do for yourself.
It’s often the little things that add up. Many people living with stage 4 blood cancer experience profound fatigue that’s nothing like normal tiredness; it’s a deep, overwhelming exhaustion that sleep doesn’t always fix. On top of that, things like nausea, sore mouth, and changes in taste can make eating feel more like a chore than a source of pleasure.
Another common challenge is low blood counts. This can increase vulnerability to infections or lead to anaemia, which often brings a familiar feeling of weakness, dizziness, or breathlessness, adding to the strain of daily life. You can find out more about the connection between anaemia and cancer in our detailed guide. Dealing with these physical hurdles, alongside the emotional strain, is why having a good support system is so vital.
Managing these physical challenges, while also coping with the emotional weight of the illness, highlights why a strong support system is so essential. Practical help, emotional encouragement, and open communication with your care team can make a meaningful difference in maintaining quality of life.
Gaining a sense of control often starts with small, practical steps. It’s about listening to your body and making simple adjustments that can soothe discomfort and help you conserve your energy while living with stage 4 blood cancer.
Here are some simple strategies that many people find helpful during this time:
Alongside these strategies, simple, practical aids can provide enormous comfort during the challenges of stage 4 blood cancer. Sometimes, it’s the small, tangible things that feel like a warm hug in the middle of a tough day.
A thoughtfully put-together care parcel can be very helpful. Items such as a soft blanket, soothing lip balm for dry lips, anti-nausea sweets, or a gentle, fragrance-free moisturiser are not just items; they are gestures of care that can provide immediate physical and emotional relief.
These small comforts are a direct answer to the daily struggles of treatment. They offer a sense of being cared for and understood, tackling practical problems from skin sensitivity and nausea to feeling uncomfortable during long hospital visits. By reducing these little discomforts, you can conserve more of your energy for what truly matters: your healing, resilience, and spending time with the people you love.
A stage 4 blood cancer diagnosis can feel incredibly isolating. But one of the most important things to know is that you don’t have to go through this alone. Building a strong support network is one of the most practical and powerful steps you can take. It provides both emotional strength and real, day-to-day help when you need it.
It all starts with your healthcare team (your oncologist, specialist nurses, and other professionals). They are your primary partners throughout treatment, because appointments can sometimes feel overwhelming, and it's easy to forget the questions you wanted to ask. A simple way to stay prepared is to keep a list of questions in a notebook or on your phone, so you’re ready whenever you meet with your doctor or specialist nurse.
Beyond the hospital, your support circle includes family, friends, and sometimes, professional counsellors. Each person has a unique role to play. Don't be afraid to tell your loved ones exactly what you need. Being specific makes it much easier for them to help, whether it's a ride to an appointment, a home-cooked meal, help with housework, or simply sitting quietly with you when you don’t feel like talking.
Equally important is finding a community of people who truly understand what you're going through, whether through support groups, online communities, or fellow patients, which can make a profound difference. It's a gentle reminder that you are not alone in your feelings or your fears.
Speaking to a professional therapist or counsellor can also make a real difference. It gives you a confidential space to work through the incredibly complex emotions that come with a cancer diagnosis, fear, anger, sadness, or simply feeling overwhelmed. They can teach you coping strategies to manage the anxiety and stress, which is beneficial for both you and your family.
The number of people affected by blood cancer globally is significant, with hundreds of thousands newly diagnosed each year. While healthcare systems are improving at early diagnosis, a stage 4 diagnosis can still feel daunting. This is where organisations like Cancer Care Parcel come in, turning daunting statistics into real, tangible support. They provide curated care parcels designed to ease treatment side effects and offer practical guides on palliative options. You can learn more about the latest research shaping these challenges in this piece from Blood Cancer UK.
Connecting with established charities and organisations is one of the best ways to find reliable information and a real sense of community. These organisations offer everything from support helplines and local meet-up groups to online forums, expert webinars, and practical advice.
Here are some of the most trusted names to explore:
When you’re told you have stage 4 blood cancer, it’s completely normal to be concerned, and your mind racing with urgent questions. Let’s walk through some of the most common questions people ask. Hopefully, this will bring a bit of clarity during a confusing time.
This is often the first and biggest question on anyone’s mind, and the honest answer is no, stage 4 blood cancer is not always a terminal diagnosis. When it comes to blood cancer, the term 'stage 4' simply indicates that the cancer has spread widely throughout the body. It does not automatically mean it's incurable.
In fact, many advanced blood cancers, like certain types of lymphoma, respond remarkably well to treatment and can often be cured. For others, such as multiple myeloma, treatment can effectively turn the illness into a manageable, chronic condition, allowing patients to live well for many years. Your prognosis is unique to you, depending on the exact type of blood cancer, your general health, and how your body responds to treatment. The best person to give you a clear, honest picture of your specific situation is your oncology team.
Deciding whether to continue working after a stage 4 blood cancer diagnosis is a deeply personal choice, and there’s no right or wrong answer. It really comes down to your treatment plan, the symptoms you're managing, the physical demands of your job, and frankly, how you feel from day to day.
For some, work provides a much-needed sense of normality and routine. They might make adjustments by arranging for flexible hours, working from home, or reduced responsibilities. Others may find it necessary to step away completely to focus on their health and recovery.
The best approach is to have an open conversation with your employer about what’s possible, and always talk to your medical team about managing symptoms in the workplace. Organisations like Macmillan Cancer Support in the UK offer excellent, specialised advice on work and financial matters during cancer treatment.
Supporting a loved one with stage 4 blood cancer is a marathon, not a sprint. The most meaningful support is often a blend of practical help and quiet emotional presence. Offering to handle specific, everyday tasks can make a huge difference, such as cooking meals, doing the weekly food shopping, driving them to hospital appointments, or helping with household chores. These small acts can lift a heavy weight off their shoulders and give your loved one more energy to focus on treatment and rest.
Just as important is being there for them emotionally. Sometimes the most valuable thing you can offer is simply being present and listening without judgment. Some days they might want to talk, while other days they may prefer silence, so it helps to respect their need for either company or space and let them take the lead on conversations about their illness. Try to learn a bit about their diagnosis so you can understand better, but avoid giving unsolicited advice.
And finally, don’t forget to look after yourself. Supporting someone through cancer is emotionally demanding, and maintaining your own well-being ensures you have the strength to continue offering care. There are plenty of resources available for caregivers, providing guidance, emotional support, and practical tips. Don’t hesitate to use them.
We strongly advise you to talk with a health care professional about specific medical conditions and treatments.
The information on our site is meant to be helpful and educational but is not a substitute for medical advice.
Learn Key Strategies For Thriving After Cancer. Explore Holistic Approaches To Improve Well-Being During And After Treatment.
Discover how to arrange compassionate end of life care at home. Our guide explains hospice, palliative care, and practical support for families.
Discover Seven Gentle and Honest Ways to Cope With the Emotional Strain of Living With Cancer, From Creating Personal Comfort Routines to Setting Boundaries and Finding Support.