From the perspective of a doctor who has looked after many patients during their final illness, I have come to learn some of those meanings - and hope to share this perspective with the people who may be coming to experience medical care at the end of life.
End of life care in medical terms can be defined broadly as a person who is likely to die within the next 12 months1. However, amongst healthcare professionals, it is generally the final weeks or days of life that are considered. This differs from hospice and palliative care, which is the medical specialty that focuses on symptom control and ensuring quality of life for patients with long-term, progressive and incurable diseases from the point of diagnosis to the end of their life2. End of life care can be seen as a subset of palliative care - and a patient being supported by the palliative care team should not be taken to mean they are at the end of their life.
However, the definition of what end of life care really means is not limited to a specific medical circumstance or particular time course - within those four words are myriads of meaning.
It may be that to the patient, some of this meaning is lost - people at the very end of their life may have a limited awareness of their situation and spend much of their time in a state of unconsciousness.
Those four words may have been what they have been dreading to hear - the final confirmation from the doctor that the fight has been lost. To some family and friends, it may be a relief - their loved one / family members may have had a protracted struggle against a debilitating illness, which will soon come to an end. There is a broad spectrum of reaction to this news, and there is no one correct response to have. Each patient and each family are different, with their own unique circumstances.
To health care professionals, there is a deeper meaning to end of life care than simply being a phase of illness, and this rests on the recognition that this is a situation of the utmost priority that necessitates the very highest standards of care. It is the time to “get it right” - a principle that is considered sacrosanct amongst those caring for dying people.
How a loved one’s death is experienced often becomes a defining memory and is known to affect the grieving process3. It is the point that brings together all of the people important to the patient and those involved in their care. It is a moment to facilitate the patient spending as much quality time as possible with their closest family and friends. It is a time to identify their key priorities - so that the professionals can ask the question
This is true at all times in healthcare, but at no time is it more essential than at the end of life that the patient and their family members / loved ones are informed and involved. End of life care is not something that should be kept behind a shroud. It is a situation in which doctors and nurses should give appropriate transparency to ensure the identified priorities and individual needs of the patient are met.
What unifies all of those involved in caring for someone who is near the end of their life, is the desire for the person at the centre not to suffer. It is a sentiment echoed by patients, their loved one, family members, caregivers, and the professionals looking after them. Suffering at the end can be physical, psychological, emotional, or spiritual - and care at this stage involves considering all of these aspects.
There is
This unified goal gives end of life care a focus. It helps to ensure that distress is minimised - which is the expertise of palliative care clinicians. Of course, no doctor can take away the pain of losing a loved one, but what doctors and nurses at the this stage of life can do is alleviate this suffering by ensuring a comfortable and dignified death.

To recognize that a patient has reached the final stages of life is solemn and serious. It takes appropriate precedence above all other matters of the ward. The first time I was involved in caring for a patient at the end of life, the significance struck a deep chord within me and has resonated since - leading me to pursue a career in palliative medicine. It was so clear how important what we had been entrusted with was, and the urgency of “getting it right” was so apparent.
The gravity of the end of life phase of a person’s illness means that the language used in the situation can carry extra significance. It is essential to be mindful of this. It is common to describe patients with terminal illnesses as fighting a battle - the risk with this is that reaching the end of life can be seen as “losing”4.
Each patient suffering from a chronic disease should be commended for their strength. It is no failure of either the patient or healthcare if the illness is not one that can be lived beyond. A change in treatment priority from curative to comfort should maintain the highest standards. If an illness cannot be cured, the patient can still be treated, bringing relief to them and their loved ones. There is no such thing as “giving up” in chronic illness – whether that be the patients or the people looking after them.
It is the care given to a patient, and those important to them, in the final phase of a terminal illness. It is arguably the most crucial part of a patient’s journey. A time at which it is most vital to provide the patient and their loved ones the best possible experience of healthcare, to bring comfort at what will be the most difficult of times they experience. It is a time to “get it right”, - which is achieved through clear and open communication, maximizing comfort, and maintaining the highest standards of care through identifying and meeting the priorities of a patient and their family members and people closest to them.
The battle to me of terminal illnesses is not in defeating an illness which by its nature cannot be overcome, but in ensuring that we help to give the patient and family the best possible experience of the final phases of the illness - if we can achieve that, and give people peace and comfort, we have won a victory against illnesses that are determined to take those things away.
The end of someone’s life is not a failure of medical treatment or of personal resilience; it is an opportunity to ensure the very best care.
It is an honour to be given this opportunity and to share in these moments.
We understand that this is a very hard time for friends, family, and loved ones. Your emotional needs as well as those of the dying person need to be addressed. There may be symptoms in their last days that you are trying to address, such as loss of appetite. You may be wondering how to provide comfort as the person you know is approaching the end or may feel you are no longer able to help. All your feelings are valid and usual and it may take a long time for your emotions to settle.
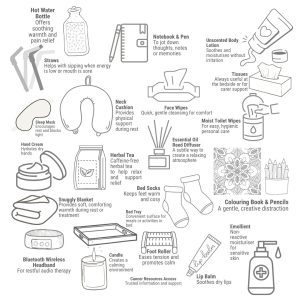
There are some simple things you can get to make it easier for the dying person. These are simple items that you should be able to obtain easily such as
STRAWS: useful when it becomes hard to drink.
MOIST TOILET WIPES: for when they are not mobile.
FACE WIPES: To stay fresh and clean.
E45 CREAM: To help with dryness.
And if you can't be there we have a Terminal Cancer Care Package, with the above items and more-no profit is made on this item.
We strongly advise you to talk with a health care professional about specific medical conditions and treatments.
The information on our site is meant to be helpful and educational but is not a substitute for medical advice.
It's My Mission And Duty To Raise Awareness As Much As I Can So No One Else Experiences This Illness That Takes So Much From You.
Cancer affects more than the body. Learn about the emotional labour carried by patients and carers, and why sustainable support and realistic expectations matter during treatment.
Care During Cancer Treatment: Read Matthews Story On How A Cancer Care Parcel Donated To Him Helped During His Cancer Treatment.